Skin Lesion Photography
Post date: 09/04/2013 | Time to read article: 3 minsThe information within this article was correct at the time of publishing. Last updated 18/05/2020
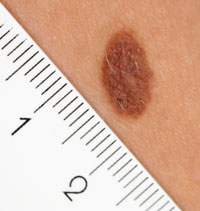 MPS statistics suggest that a case relating to the delayed diagnosis of melanoma is opened every two weeks. Dr Pawan Randev argues that skin lesion photography is a way of improving feedback on dermatology referrals
MPS statistics suggest that a case relating to the delayed diagnosis of melanoma is opened every two weeks. Dr Pawan Randev argues that skin lesion photography is a way of improving feedback on dermatology referrals
GPs are frequently confronted by patients who are anxious about skin lesions. Our confidence in diagnosing and managing pigmented lesions depends on our experience. This article describes a system of feedback on your own referrals, which is educational and targeted.
When a patient presents with a pigmented lesion, one of the key questions for the GP is whether to refer. Suspected malignant melanoma and squamous cell carcinomas should be referred on the Two Week Wait Pathway. Patients will be seen within two weeks, but the correspondence and histology may take a further four weeks to return to the practice.
Over this period, a full-time partner may have seen more than 600 further patients. Thus, the reply letter to the referring GP is difficult to relate to the original lesion seen. Within our practice, we have developed a system, whereby any lesion that merits urgent referral is also photographed and the image uploaded to the patient’s clinical records. In this way, when the letter from the clinic is received, it can be viewed alongside the clinical image that prompted us to start the referral process.
From an educational point of view, this gives visual feedback on a visual decision. It allows informed discussion with colleagues around the original decision to refer. The lesion is context sensitive, ie, working in an area of patients with pigmented skin will give you images of that skin tone. By read coding the images as “skin lesion photography”, the photographs become searchable. This has become a valuable teaching resource for our trainers.
Suspected malignant melanoma and squamous cell carcinomas should be referred on the Two Week Wait Pathway
The same principle applies to lesions that are being excised. Many GPs have inadvertently excised lesions that turned out to be melanoma or squamous cell carcinoma. If a lesion is to be excised, a photograph can be taken pre-surgery and placed in the medical record. Thus, outcomes can be reviewed and discussed with colleagues. This represents good clinical governance and has been used for appraisal discussions.
Other uses include monitoring of effectiveness of acne treatments, discussing unusual or unclear dermatology conditions with GP colleagues and reviewing outcomes of hospital-based treatments, eg, PUVA for psoriasis.
Patients appreciate the additional value and have all agreed to this when the purposes of the photograph are explained. Many already have smartphone photographs of their lesions. When the image is seen together there is a unique opportunity to educate the patient on features of melanoma that we are looking for. Patients sign a consent form that allows sharing of the image by clinicians for teaching and learning purposes.
Some GP computer systems allow sharing of the image with secondary care. It is possible to attach the image to choose and book referrals. We have found that there is variable access to computers and the choose and book system by consultants. This systematic change is an educational feedback loop for primary care, which can enhance our future decisionmaking on pigmented lesions.
The photographs are taken using a standard digital camera (Panasonic Lumix or Canon Ixus). Within the image we include a patient label. The Brother label printer stickers include a 4cm barcode, which acts as a ruler. It also generates a date. The cameras all have a standard macro mode and flash.
By read coding the images as “skin lesion photography”, the photographs become searchable. This has become a valuable teaching resource for our trainers
The whole process of taking the photograph and uploading to EMIS Web takes me less than two minutes. This can be achieved within a consultation. However, our healthcare assistants have also been trained in taking photographs and uploading the images to the record. The images are treated in the same way as we input any documents, as an attachment to the clinical record. The process is similar to adding attachments to email and is the routine for attaching letters to the clinical record.
It is notable that our nursing colleagues in the community have been using photography to monitor wound healing for a number of years.
The aim is to provide educational feedback for referring doctors so that we can assess and share our educational needs with colleagues in primary care. We have no evidence that this will reduce referral rates. However, it does stimulate discussion and debate within the primary care team and maintains knowledge of referral criteria based on our own activity. It is a simple, efficient addition to current clinical activity, which can be delegated to nonclinical staff.
Patient feedback has been very good. No-one has declined the offer of photography. Most patients are impressed to see their skin lesion on screen. There have been no refusals.
In our practice this has proven to be an effective, stimulating and efficient educational process. Further details, including a consent form and Powerpoint presentation are available on our practice website.
Read about the risks of missed melanoma in Dr Richard Stacey’s feature ‘Watch out for the melanoma black spot’
