Getting to grips with fit notes
Post date: 29/08/2017 | Time to read article: 6 minsThe information within this article was correct at the time of publishing. Last updated 18/05/2020
A common question in general practice: “Ms P’s fit note runs out on Monday – can you do her another one?” Your answer should be considered carefully as the following case illustrates, explains Dr Rachel Birch, GP and medicolegal adviser at MPS
Dr A, a GP registrar, received the message “Ms P’s fit note runs out on Monday – can you do her another one?” at 4pm on a busy Friday afternoon. Her GP trainer, Dr S, was doing the ‘duty doctor’ session at the main premises, but the request was passed to Dr A as Dr S was undertaking an urgent home visit.
Dr A was told that Ms P had been on the phone and had appeared worried – she had told the receptionist that she wasn’t sure if she should return to work or not, but that her fit note was due to run out on Monday and she would be in trouble with her boss if she did not hand another note in. She asked to pick up the fit note at 5.30pm.
Dr A had never met Ms P before. She looked in her medical record and noted that Ms P had been seeing Dr M, the senior partner, for depression and anxiety. She appeared to have had three fit notes issued in the last four months. The notes were fairly brief and although Dr M had documented that Ms P had “greatly improved” there was no clear advice regarding her job, or a return to work.
Dr A realised that she needed to make an assessment of Ms P before completing a fit note. Dr M was out of the practice for the day, so she could not obtain any further background information about the patient. She spoke with Dr S, but he had not previously met the patient.
Dr A tried to contact Ms P by telephone, but was unable to reach her. She asked the receptionist to keep trying to contact her to explain that Dr A was unable to issue a fit note without reviewing her and to organise for Ms P to come down to the practice that afternoon for a review appointment. The receptionist was unable to reach Ms P on the telephone.
I find it difficult when patients ask for fit notes for less than seven days of sickness even though legally they don't need one.
Dr A could see that Ms P had improved clinically since she was first off work four months ago. However, with limited time to review her, and not having met her before, she explained to Ms P that it would be better to see Dr M on Monday morning. Ms P reluctantly agreed to this.
Ms P saw Dr M on Monday morning and they discussed her potential return to work. Ms P had thought that she only had two options: to be off work, or back at work full time. However, Dr M explained to her that after a long period of illness a phased return to work was often a good idea. They agreed that a reasonable plan would be for Ms P to go back to work for the mornings only initially, building up to her full hours over the following four weeks or so. He completed the fit note to state that Ms P may be fit to work if her employer could facilitate a phased return to work. He advised Ms P that he would be happy to discuss his recommendations with her boss and she consented to this and said that she would ask her boss to contact Dr M.
The following day Ms P’s boss spoke with Dr M on the telephone. She told him that she appreciated the chance to speak to Dr M, so that arrangements could be put in place to support Ms P and her return to work. Ms P went back to work the following week. Five weeks later Dr M and Dr A received a letter of thanks from Ms P who had made a successful return to work and was continuing to improve from her depressive illness.
Fit note guidance
The Department of Work and Pensions offers guidance on the completion of the Statement of Fitness to Work (fit note).1 The patient should be assessed for fitness to work and, in doing so, doctors may choose to undertake face-to-face consultations, telephone consultations or consider reports from other doctors or healthcare professionals.
The Department of Work and Pensions offers guidance on the completion of the Statement of Fitness to Work (fit note)
The General Medical Council (GMC) expects doctors to be honest and trustworthy in all written documents, including in fit notes. They state that doctors should ensure that any documents they sign are not false or misleading, and doctors must take steps to verify the information in the documents.2
Good practice points:
Dr A had not met Ms P before, and the notes were scanty, so she tried to arrange to review the patient herself prior to issuing a fit note.
Dr A did not feel pressurised into issuing a fit note, despite the time pressure, but instead arranged for the patient to be reviewed by her usual GP, Dr M, the following working day.
Dr A was sympathetic and supportive to Ms P and offered to see her after hours as she had attended the surgery in some distress.
Dr M took time to reassess Ms P and felt that she would be fit to return to work with certain modifications to her working hours for the next few weeks. He used the fit note constructively with Ms P, to illustrate the options available to her and to support her decision to return to work. He offered to liaise with her employer, and did so, which was appreciated by both Ms P and her employer, and ultimately contributed to a successful return to work.
Three-second survey – Fit notes
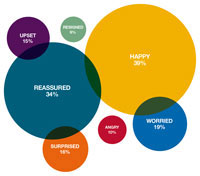
MPS conducted a short survey to find out about most patients’ reactions to fit notes. According to our sample, on average 1 in every 13 patients is issued with a fit note. This bubble chart highlights patients’ reactions to fit notes:
Useful links
References
- Department of Work and Pensions, Getting the most out of the fit note: GP guidance (March 2013)
- GMC, Good Medical Practice, par 71 (April 2013)
Vox pops
We asked GPs about fit notes. Here’s what they said:
"It is a farce that the ESA appeals take nine+ months and we are obliged to provide notes to cover this when 95% should be seeking employment. There is a downturn in people seeking notes (a good thing), although there are many of my patients who are exploiting our over generous benefit system – it would be nice if there was an anonymised whistleblowing hotline where we could give our professional view on those who ‘play the system."
"I find it difficult when patients ask for fit notes for less than seven days of sickness even though legally they don t need one."
"Fit notes work best with large companies with occupational health or HR input. Smaller companies can find it difficult to find alternative work roles, or so my patients tell me. They seem to be useful in the return to work phase when someone has been off work for a number of weeks."
"The previous sick notes had the ability to certify a patient as fit for work. With the current form if an unfit for work statement is made and the patient s condition improves, there is no facility to state is fit you can only put may be fit."
"Little has changed in practice in terms of the number of ‘sick notes’ issued by GPs and sick notes’ continue to be a thorny issue in the practice of most GPs. Not infrequently, the main reason for issuing a sick note is to avoid a conflict with the patient, rather than for purely clinical reasons."
