Good night and good luck
Post date: 04/01/2012 | Time to read article: 5 minsThe information within this article was correct at the time of publishing. Last updated 18/05/2020
 Dr Kyle Stewart and Dr Pippa Woothipoom explore how junior doctors can get the most out of their on-calls
Dr Kyle Stewart and Dr Pippa Woothipoom explore how junior doctors can get the most out of their on-calls
Ask any final year medical student about their biggest worry about becoming a doctor and they will answer “on-calls”. Here is the advice we wish we’d had when we started doing on-calls.
Seek senior support
The main worry about on-calls is being responsible for someone dying or becoming really unwell. The truth is, yes there are sick people in hospital, and yes, you will have to see them – but the important point is that you are not the only doctor in the hospital. Senior doctors are there for advice – be proactive in seeking it.
Assessing sick people
After reading a patient’s history consider:
- Why are they in hospital?
- What has happened to them since they have been in hospital?
- Have they got a significant past medical history?
- What investigations you could rule in/out
- Reassessing patients when you have done your investigations (bloods, x-rays etc).
If you’re still unsure after doing this, whomever you handover to will appreciate that you have done appropriate investigations.
Use time efficiently
If you are called to the wards to write up fluids call the ward first and ask them to get the fluid chart, so it is ready when you get there. It is a good idea to try and persuade the ward to get together any other jobs that need doing so you can do them in one batch.
Discussing patients with their family
This can be difficult if you don’t know the patient. Have a look through the patient’s notes and talk to the nurse to find out more. If you still do not feel like you are in a position to answer these questions, do not feel pressurised to do so. This is often best left to the day team who know the patient.
Discussing patients with their family is often best left to the day team who know the patient
What to expect on-call
In January 2010, we audited the jobs medical or surgical F1 doctors were asked to do on-call in Torbay Hospital. The total jobs are shown in the table below.
During the week in Torbay Hospital, there is:
- one medical F1 (5pm – 11.30pm)
- one surgical F1 (5pm – 10.30pm)
At the weekend there are:
- three medical F1s who work different shifts 9am – 5pm, 10am – 10pm, 11.30am – 11.30pm
- two surgical F1s who do 9am – 6pm, 3.30pm – 10.30pm.
Most common on-call jobs
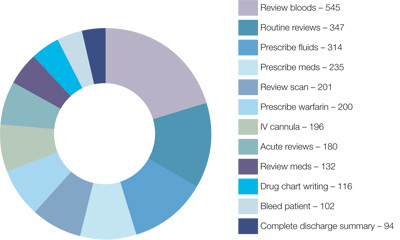
Advice on most common on-call jobs
Reviewing bloods
The majority of F1s’ on-call time is spent reviewing blood tests. The majority of these are required at the weekend as practitioners need daily reviews of common things, like U&Es, HB and inflammatory markers.
Prescribing fluids
Prescribing fluids is a very common job. This is mostly maintenance fluid for people with insufficient oral intake to match their needs. Always check the patient’s renal function before prescribing fluids, in particular their sodium and potassium. Before speeding up fluids, or giving fluid challenges for patients who are becoming unwell, remember to assess their fluid balance and past medical history. Fluid overloading a patient can be just as dangerous as leaving them dehydrated.
Contrary to what people may tell you, diazepam is not always the answer
Prescribing meds
Often this is night sedation, eg, zopiclone, changing from IV to oral antibiotics, or prescribing a new patient’s regular medication. Whatever the reason, make sure you know the medication and why you are prescribing it. If in doubt ask. Do not prescribe just because a nurse tells you to. Be particularly careful when prescribing sedating drugs to elderly and confused patients. Contrary to what people may tell you, diazepam is not always the answer.
Reviewing scans
This means reviewing chest x-rays and looking for consolidation or fluid overload. Other common investigations include ECGs, abdominal films (especially if you’re a surgical F1) and bone x-rays. If you are unsure, ask a senior colleague. Also, be sure to check that the name on the scan matches that on the patient’s wrist bands.
Prescribing warfarin
There is no need to check a patient’s INR four or five times a week if it is stable. Take care in prescribing warfarin if it could be affected by antibiotics and other medications.
Acute reviews
Take your time when reviewing someone who is becoming unwell. Use stepwise approaches like ABC for airway, breathing, circulation and remember to call for help if you need it. You are not expected to look after every sick, dying patient in the hospital on your own!
Reviewing medications
Rewriting drug charts is the most unpopular F1 job at our hospital. This is a job that should be done by the day team; it is not fair to ask an on-call doctor to do this. Similarly, completing discharge summaries should not be the role of an on-call doctor.
Reviewing patients for discharge
There should be a clear plan in the notes on the criteria the patient must meet before discharge. If you are unsure, do not send the patient home; review the patient and discuss with a senior.
Rewriting drug charts is the most unpopular F1 job at our hospital
Helping colleagues on-call
You are part of a team: here are some things to think about:
- Make sure drug charts have plenty of space for overnight or over the weekend; rewrite them yourself if they don’t.
- If you want a patient reviewed over the weekend, write a clear plan in the notes. Be precise. A clear instruction like “if haemoglobin less than 7, transfuse 3 units and re-check tomorrow” is easier to follow than “if hb low, give blood”.
- Try to order fewer bloods over the weekend so there are fewer results to be checked.
- Do your routine bloods earlier in the day, so you will get the results sooner.
- Ensure fluids are prescribed for overnight so a doctor isn’t called to the ward to write-up maintenance fluids.
- Have a ward round with your nursing staff before you go. Make sure they haven’t got any issues or questions; if they don’t ask you now, they’ll phone an on-call doctor who, again, will not know the patient.
My first on call
By Dr Kyle Stewart
When I did my first on-call, I remember picking up the on-call phone, and being petrified when it went off immediately.
A post-op patient had become drowsy on one of the surgical wards. I ran to the ward, Oxford Handbook at the ready, racking my brain to remember the causes of drowsiness. When I got there the patient had her eyes closed. As I ran over, my heart was pounding. When I got to her bed I shook her and shouted across the bay “Can I have some assistance, please?”
As I frantically searched for anyone, I turned back to the patient, who was wide awake and staring up at me. “Is everything alright dear?” she calmly asked, as two nurses flew over to the bay. They had seen me grab the poor 92-year-old, who was recovering from hip surgery. It turned out she was tired from her surgery and wanted a nap.
That day I learnt that when people are asleep they are unresponsive unless you wake them up! Always remember to think of common things first and be systematic in your approach. You will be able to think much clearer when you aren’t panicking.
A final word
Being on-call will be intimidating as you will face unfamiliar situations that you have not been trained to deal with. Just remember to take your time, assess the situation and see what you can do. Remember to call for senior support early if you think a patient is deteriorating. Use your on-call time to become familiar with new topics and shadow your seniors.
You will soon realise that you learn more on-call than at any other time
Treat it as a unique learning opportunity that could boost your CV by providing interesting topics for CBDs and mini-CEXs. You will soon realise that you learn more on-call than at any other time. Good night and good luck!
Dr Woothipoom is an F2 in elderly care and Dr Stewart is an academic F2 in gastroenterology at Torbay Hospital in Devon. Thanks to acute care consultant Dr Nigel Benjamin for his help with this feature.
