Learning from Cases: Haematology
Post date: 14/04/2026 | Time to read article: 3 minsThe information within this article was correct at the time of publishing. Last updated 27/04/2026
• Read this resource to: Understand the claims environment in haematology
• Access tailored advice and key recommendations to help you reduce risks in the future
Expert advice for haemotologists
Haematology is a unique field where clinical skills and laboratory work help provide a holistic approach to patient care. Haematologists are often required to provide input on complex cases for other specialties, so the advice you receive needs to be equally specialised.
As a Medical Protection member, you benefit from more than 130 years of experience defending doctors and other healthcare professionals. That isn’t just a number – it’s more than 13 decades of specialist expertise that we use to protect you long into the future.
The medicolegal team at Medical Protection have reviewed a range of haematology cases to identify common causes of claims and the different types of cases involved. Their analysis aims to keep you informed about current trends and provide useful insights to help you to protect yourself throughout your career.
Introduction
Haematology is a fairly common source of medicolegal cases, including complaints. Often this is due to the chronic nature of the condition or the complexities of patients who may require specialist input to stabilise them prior to receiving other medical care.
Haematology cases at Medical Protection are dominated by inquests. This may be due to the complicated shared care and multidisciplinary nature of haematology cases. Or there may also be circumstances where a patient’s haematological condition has contributed to their death. On occasion, further information is needed from a haematologist to understand a particular condition or treatment.
Haematology has seen a large rise in requests for assistance with public inquiries. In these cases, Medical Protection can offer valuable support to members and provide expertise in what can be a lengthy and stressful process. Other reports that may be required by haematologists include patient safety incident response framework (PSIRF) reports whereby an in-depth review of a clinical incident is undertaken to learn from the incident.
As NHS Resolution manage claims relating to NHS patients in secondary care, the low number of claims Medical Protection assists with indicates that most haematological care is provided within an NHS setting, as opposed to privately. This is a different landscape compared to some other medical specialities, for example dermatology, where more patients access care privately.
The value of a settled claim will often include compensation for care and loss of earnings if applicable, in addition to an award for the damage that resulted from a breach of duty. The value of each claim varies enormously, with our highest haematology total case payment considered in this analysis being just under £200,000. This includes claimant damages, costs, and legal costs.
As a haematologist, you work in a varied environment where patients may be under the care of a number of specialists and other healthcare professionals. This can understandably contribute to a more complicated landscape for your work. We also know, following feedback from members, that experiencing a medicolegal case can be incredibly stressful. At Medical Protection, we want to share our knowledge, experience, and expertise with you so we can provide invaluable professional support when you need it most.
Analysis
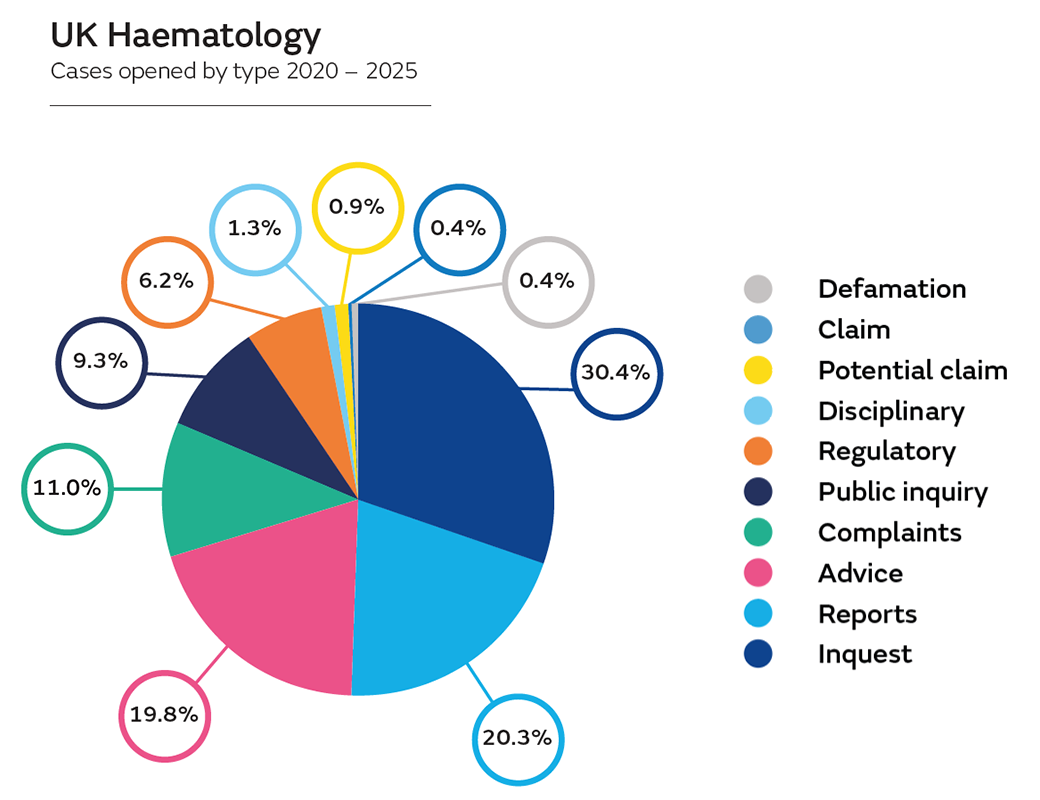
We have analysed the support we’ve provided to UK-based haematologists between 2020 and 2025 – in excess of 200 cases. We have supported our haematology members in a full range of situations, including:
- inquests
- complaints
- public inquiries
- General Medical Council (GMC) investigations
- local disciplinary procedures
- claims – demands for monetary compensation that embody allegations of negligence
- potential claims – intimations from a claimant of a possible claim for compensation
Read related case report – A guiding hand through the inquest process
Read related case report – Case closed after a pause for reflection
Haematology in the UK: top tips to minimise risk
Please note this is not an exhaustive list of recommendations, but key learning points from our analysis.
- Be particularly careful when sending documents including patient information and ensure they are sent to the intended recipients. Medicolegal advice can be sought for third party requests for confidential patient information.
- Some complaints brought by patients or relatives follow dissatisfaction with the manner and attitude of their clinician. Pay attention to how you may be perceived during discussions and ensure time is taken to explain the situation and answer any questions.
- Accurate and clear documentation, which often may need to be relied on years after the event, is the cornerstone of any medicolegal defence. Be aware that you may be asked to write a statement, including in relation to claims, inquests, and complaints about your practice months or even years after an event, and ensure that your contemporaneous record keeping would allow you to give a comprehensive account of your involvement.
- Ensure you are fully indemnified to carry out the full scope of your practice in the UK, including medicolegal or expert witness work.
- Seeking advice early when confronted with a situation that is challenging or complex from a medicolegal perspective can reduce the chance of a complaint escalating or even arising in the first place.
About the author
Dr Emma Green is a medicolegal consultant with a career in emergency medicine before joining Medical Protection in 2016. She returned to the frontline to assist during the COVID-19 pandemic. She has worked across a range of departments at Medical Protection, including claims, case handling, and more recently in underwriting.
